PTSD Self-Help: PCL5-Based Recovery Strategies
March 10, 2026 | By Camila Jensen
After taking a PCL5 assessment and receiving your score, the journey toward healing truly begins. Understanding your PTSD symptoms is just the first step in a longer process. Managing these symptoms effectively is where real progress happens. Many people feel overwhelmed after they start your test and see their results.
This comprehensive guide goes beyond basic grounding techniques. It provides advanced, evidence-based self-help strategies organized by the specific symptom clusters found in the PCL5 assessment. Are you ready to turn your PCL5 results into a clear plan for recovery? By learning how to target specific symptoms, you gain practical tools to take active steps in your healing journey.

Understanding Your PCL5 Results and Symptom Clusters
The first step to recovery is knowing what you are dealing with. The PCL5 is not just a list of questions; it is a map of your current mental state. When you use a PCL5 online test, you are looking at how trauma currently affects your life. Understanding the data behind your score helps you choose the right tools for management.
Decoding Your PCL5 Score: What the Numbers Mean
When you complete the 20 questions on the checklist, you receive a total score between 0 and 80. A higher score generally indicates a higher severity of symptoms. Typically, a score between 31 and 33 is used as a "cut-point" to suggest that a person may meet the criteria for PTSD.
However, your score is more than just a single number. It tells a story about which areas of your life are most impacted. For example, a high score in the "Intrusion" category means you likely struggle with memories or nightmares. Understanding these nuances allows you to prioritize your self-help efforts where they are needed most.
The Four Symptom Clusters: A Framework for Management
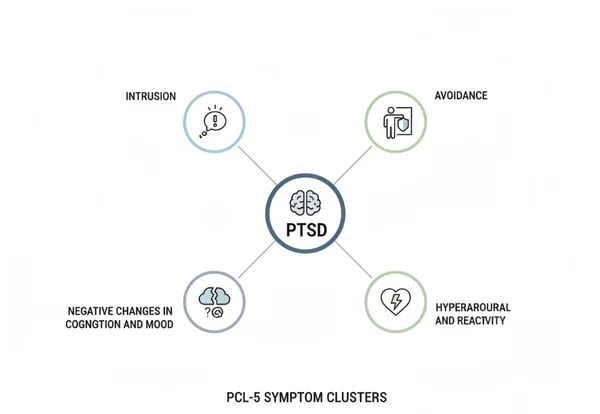
The PCL5 organizes 20 symptoms into four distinct categories, or "clusters." These clusters are based on the DSM-5 standards for diagnosing PTSD. They include:
- Intrusion: This involves unwanted memories, flashbacks, and nightmares.
- Avoidance: This is the effort to stay away from people, places, or thoughts that remind you of the trauma.
- Negative Changes in Cognition and Mood: This includes feelings of guilt, fear, or a loss of interest in activities.
- Hyperarousal and Reactivity: This covers being "on edge," irritable, or having trouble sleeping.
By viewing your symptoms through these four lenses, the problem becomes more manageable. You can stop trying to fix everything at once and focus on one cluster at a time.
Personalizing Your Approach to Recovery
No two people experience trauma in the same way. One person might struggle deeply with sleep, while another might struggle with constant negative thoughts. This is why a "one size fits all" approach rarely works for PTSD.
Effective self-help requires you to tailor your strategies to your individual experience. If your results show high scores in hyperarousal, you should focus on physical relaxation. If your scores are higher in avoidance, your focus should be on gradual reconnection. You can take the test to see which cluster is currently your biggest challenge.
Managing Intrusion Symptoms (Flashbacks and Nightmares)
Intrusion symptoms are often the most distressing part of PTSD. These symptoms make it feel as though the traumatic event is happening again in the present moment. Managing these requires techniques that pull your brain back into the safety of "now."
Grounding Reimagined: Advanced Techniques for Flashback Interruption
Most people have heard of "grounding," but advanced grounding goes deeper. One powerful method is the 5-4-3-2-1 technique. When a flashback starts, name five things you see, four things you can touch, three things you hear, two things you can smell, and one thing you can taste.
To make this more effective, try "dual awareness." This means acknowledging that a memory is present while also naming a physical fact about your current environment. For example, say out loud: "I am remembering a scary time, but I am also sitting in a blue chair in my living room in 2024." This helps your brain distinguish between the past and the present.
Trauma-Informed Journaling: Rewriting Your Narrative
Intrusive thoughts often feel like broken records. Journaling can help "process" these loops. However, it is important to use a structured approach. Instead of just writing about the pain, try "narrative reframing."
Write down an intrusive memory. Then, write down three things you know now that you didn't know then. Write about the fact that the event ended and you survived. This helps the brain move the memory from an "active" threat to a "historical" event.
Nightmare Management: Sleep Strategies for Restorative Rest
Nightmares can make you afraid to go to sleep. One evidence-based strategy is "Imagery Rehearsal Therapy" (IRT). During the day, think of a recurring nightmare and write it down. Then, rewrite the ending to something neutral or positive.
Before bed, spend five minutes visualizing the new, changed version of the dream. This simple exercise can reduce the frequency and intensity of nightmares over time. Combined with good sleep hygiene—like keeping your room cool and dark—you can slowly reclaim your night.
Addressing Avoidance and Numbing Behaviors
Avoidance feels like a safety net, but over time, it becomes a cage. It prevents you from living a full life. Addressing these behaviors is about slowly expanding your world again without overwhelming your system.
The Gradual Exposure Framework: Small Steps Toward Reconnection
You cannot stop avoiding everything all at once. Instead, create a "ladder" of things you avoid. At the bottom of the ladder, put something that makes you slightly uncomfortable. At the top, put the thing you fear most.
Start at the bottom. If you avoid grocery stores, try going for just five minutes during a quiet time. Once that feels okay, try ten minutes. This gradual exposure teaches your brain that these situations are not actually dangerous today. Using the free PCL5 test every few weeks can show you how your avoidance scores are dropping as you climb your ladder.

Reclaiming Activities: Rediscovering Joy Despite PTSD
PTSD often robs people of their hobbies. You might feel "numb" or like you don't care about things you used to love. To fight this, you must schedule "joyful" activities even if you don't feel like doing them.
This is called behavioral activation. Choose one small hobby, like gardening or listening to music. Do it for 15 minutes a day. Don't wait to "feel" like it. The feeling often comes after the action. Over time, these small actions help break the cycle of emotional numbing.
Mindfulness for Emotional Engagement: Moving Through Numbness
Mindfulness is often misunderstood as "clearing the mind." In trauma recovery, mindfulness is about "noticing." If you feel numb, notice the numbness. Where do you feel it in your body? Is it a heaviness in your chest or a coldness in your hands?
By simply observing the sensation without judging it, you take away its power. This helps you slowly move through the numbness rather than being stuck in it. It allows you to re-engage with your emotions at a pace that feels safe.
Strategies for Hyperarousal and Reactivity
Hyperarousal is like an alarm system that won't turn off. You might feel jumpy, irritable, or constantly watching your surroundings. These strategies focus on calming the physical body to signal to the brain that it is safe.
Body-Based Regulation: Somatic Techniques for Anxiety Reduction
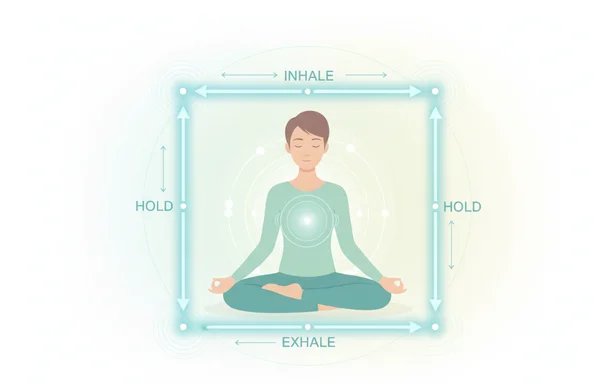
Your nervous system is "stuck" in a high-alert state. Somatic techniques can help manually reset it. One of the most effective tools is Box Breathing. Inhale for four seconds, hold for four, exhale for four, and hold for four.
Another technique is Progressive Muscle Relaxation. Starting at your toes, tense every muscle group for five seconds and then release. This physical release of tension sends a powerful signal to the brain that the "fight or flight" response is no longer needed.
Cognitive Reframing for Irritability and Anger Management
Anger in PTSD is often a "secondary" emotion. It usually hides primary emotions like fear or vulnerability. When you feel a surge of irritability, ask yourself: "What is underneath this anger right now?"
Are you feeling tired? Do you feel unsafe? By identifying the underlying need, you can address the real problem rather than reacting with anger. This reframing helps preserve your relationships and reduces the stress on your body.
Creating Safety: Environmental Adjustments for Better Regulation
Sometimes, your environment triggers your hyperarousal. You can make small changes to your home or office to help you feel safer. This might mean sitting with your back to a wall in public or using a weighted blanket at home.
The goal is to reduce the number of unknowns your brain has to track. When your environment feels controlled and safe, your internal alarm system can finally start to dial down. If you want to see how these changes affect your levels, use the PCL5 regularly to track your hyperarousal score.
Working with Negative Changes in Cognition and Mood
Trauma can change the way you think about yourself and the world. You might believe you are "broken" or that the world is "completely dangerous." These cognitive strategies help you challenge these painful beliefs.
Challenging Negative Beliefs: Evidence-Based Thought Restructuring
When a negative thought arises, like "I can't trust anyone," treat it like a hypothesis, not a fact. Look for evidence for and against that thought.
Have you met one person who was kind? Is there one person who has been consistent? By looking at the evidence, you can move toward a more balanced thought: "I need to be careful with who I trust, but some people are reliable." This shift reduces the heavy weight of global negative beliefs.

Rebuilding Self-Compassion: Healing Damaged Self-Perception
Many trauma survivors carry intense guilt or shame. You might blame yourself for what happened or for how long it is taking to "get over it." Rebuilding self-compassion means talking to yourself the way you would talk to a dear friend.
If a friend was struggling with PTSD, would you call them weak? Likely not. You would be patient and kind. Practice giving that same kindness to yourself. Healing is a difficult process, and you deserve credit for the effort you are putting in.
Rediscovering Positive Emotions: Small Steps Toward Joy
It is common to lose the ability to feel "good" emotions like happiness or excitement. You can rebuild this capacity through "savoring." When something small and pleasant happens—like a good cup of coffee or a nice sunset—force yourself to focus on it for 30 seconds.
Really feel the warmth of the cup or the colors of the sky. This "micro-dosing" of positive emotions helps retrain your brain to register pleasure again. Over time, these small moments add up to a more positive mood.
Building Your Personal PTSD Recovery Plan
Recovery from PTSD is not a straight line. It is a process of learning, practicing, and sometimes starting over. By using the PCL5 symptom clusters as your guide, you can create a targeted plan that works for your unique needs. Whether you are focusing on grounding for flashbacks or somatic techniques for anxiety, every small step counts.
Consistency is key. You don't need to do everything at once. Choose one strategy from the cluster that bothers you the most and practice it daily. Over time, you will notice your PCL5 scoring results start to change as you regain control over your life.
Remember, self-help is a powerful tool, but it is not a replacement for professional care. If your symptoms feel unmanageable or if you are in crisis, please reach out to a mental health professional.
Ready to take the next step in your PTSD recovery? Start with a confidential PCL5 assessment to understand your specific symptom profile. Start your test today and begin your journey toward a calmer, more connected life.
FFrequently Asked Questions About PTSD Self-Help Strategies
How often should I practice these self-help strategies for PTSD?
For the best results, you should practice these strategies daily. Think of them like physical therapy for your brain. Even if you aren't feeling highly stressed, practicing grounding or breathing techniques when you are calm makes them more effective when a crisis hits.
Can self-help strategies alone cure PTSD?
While self-help strategies are incredibly effective for managing symptoms, "curing" PTSD often requires professional therapy, such as EMDR or Cognitive Processing Therapy. Self-help is an excellent companion to therapy and can provide immediate relief, but a licensed professional can help you process deep-seated trauma safely.
What if these strategies make my PTSD symptoms worse?
Sometimes, focusing on symptoms can cause a temporary increase in distress. If a specific exercise, like journaling or exposure, feels too overwhelming, stop and return to grounding. It is important to pace yourself. If you consistently feel worse, it is a sign that you should seek guidance from a trauma-informed therapist.
How long does it typically take to see improvement with these strategies?
Most people begin to feel a sense of empowerment within a few weeks of consistent practice. However, significant changes in your PCL 5 score may take several months. Recovery is a marathon, not a sprint. Be patient with yourself as your nervous system learns to feel safe again.
Are there any digital tools or apps that can support these self-help strategies?
Yes, there are many tools available. Our PCL5 assessment is a great way to track your symptoms over time. Additionally, apps like "PTSD Coach" (developed by the VA) provide immediate tools for grounding and stress management that align with the strategies mentioned in this article.